Health awareness
‘Wonder Angie’ enlists her ‘super friends’ to fight oral cancer
After receiving an oral squamous cell carcinoma diagnosis, a head and neck cancer survivor finds hope by embracing science, prioritizing mental health and leaning on her work family
In 2017, Maria Angelica Rosario Marquez — or Angie, as she likes to be called — joined Merck in Colombia as a clinical data specialist. She had lost her father the year before and was looking forward to starting a new chapter. The novelty of that first year, however, was short-lived, as her mother was diagnosed with cancer in 2018.
Angie spoke to her manager, and he encouraged her to put family first. She booked a ticket to Chile and was there to support her mother and sister during the illness and her mother’s passing.
Just five months later, 34-year-old Angie was diagnosed with head and neck cancer, specifically squamous cell carcinoma of the tongue.
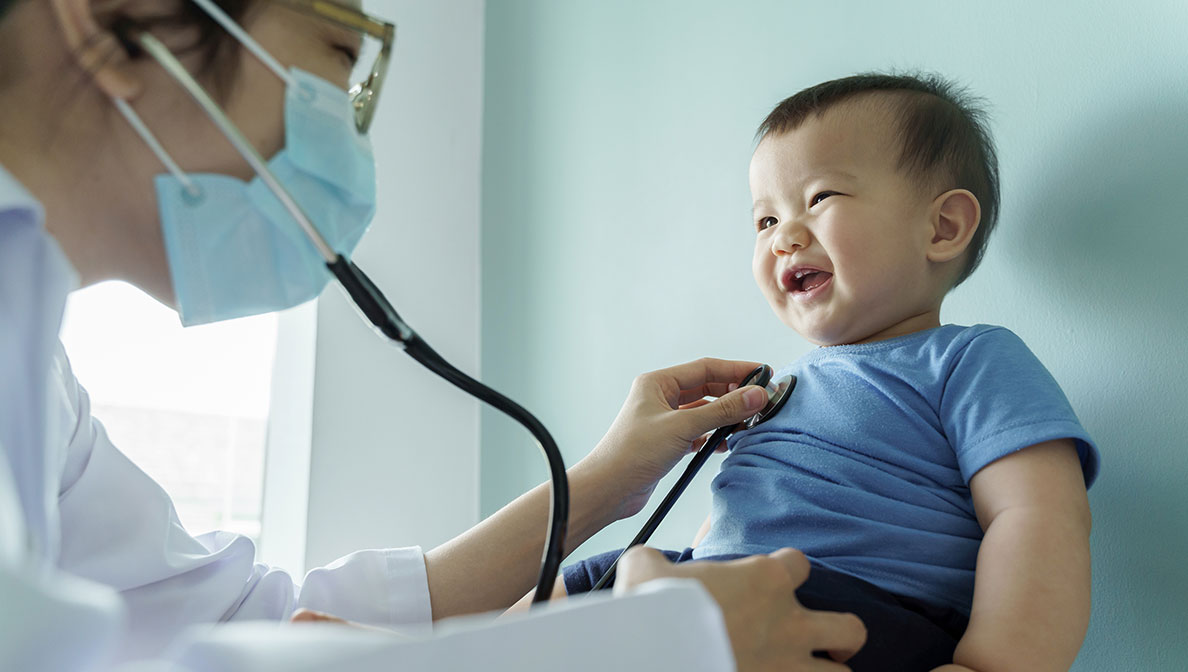
Head and neck cancer includes cancer of the oral cavity, throat (pharynx), voice box (larynx), nose (nasal cavity), sinuses (paranasal sinuses), and salivary glands. In 2023, an estimated 66,920 people were diagnosed with a head and neck cancer in the U.S. Some risk factors that can contribute to the development of head and neck cancers include tobacco use and alcohol consumption — but Angie’s disease was not linked to these typical risk factors.
It all started with pain in Angie’s tongue
When Angie developed bruxism (grinding, clenching, or gnashing of the teeth), she consulted her physician for evaluation. Angie also noticed that she was continuously biting the same spot on her tongue while she was sleeping. She assumed it was due to stress caused by the devastation of losing both of her parents and her move to a new country without her family by her side. When the pain on the right side of her tongue increased to a point that made it difficult to eat or brush her teeth, her doctor decided to take a biopsy, and in March 2019, he informed her of the diagnosis.
“It was the most frightening thing I’ve ever felt in my life,” she said.
A week later, Angie had surgery to remove the right portion of her tongue, which contained the cancerous tissue, as well as 21 lymph nodes on the right side of her neck. A further analysis of the lymph nodes showed evidence of cancer, so her oncologist followed up with a treatment plan that included three chemotherapy sessions and 30 days of radiation on her neck and tongue.
The toll of Angie’s treatment for oral cancer
Following her surgery and throughout treatment, Angie experienced a burning feeling in her mouth and throat, and it became extremely difficult for her to speak or eat — two of her favorite activities. Instead, she relied on a feeding tube for several months to receive her meals.
Though Angie was eventually able to resume eating normally, her sense of taste was impaired for a year after she finished treatment. The fact that chocolate, one of her favorite foods, tasted disgusting to her was heartbreaking.
“The doctor told me that he didn’t think I’d ever be able to speak well again. I told him that wasn’t an option because I love talking too much.”
When Angie started to feel a deep depression, she prioritized her mental health and sought treatment from a psychologist, who taught her to focus on the present. Her psychologist encouraged her to visualize herself as a strong and healthy woman.
“I always say cancer was my teacher; it taught me how to live. If you have air in your lungs, you have everything you need,” Angie said.
Strong support and a welcome party from her work family
Angie is grateful for the science and research that helped play a part in her treatment. As of her last doctor’s visit, she remains healthy with no evidence of disease. Angie credits her work family at Merck for supporting her through much of her recovery. With the recent loss of her parents, her co-workers came to her aid with powerful emotional support that helped her through the toughest times. A lifelong collector of superhero toys, Angie came back to the office to find her desk covered in dolls, figurines and other gifts. Inspired by Angie’s courage, her colleagues even gave her a super-nickname: ‘Wonder Angie.’
“I’m thankful for the science and medicine that helped save my life,” Angie said. “I can talk without pain, and that’s amazing. I can brush my teeth every day, and that’s amazing. I can eat, and that’s amazing.”
Angie’s sense of taste has returned for the most part, and she’s enjoying chocolate once again.